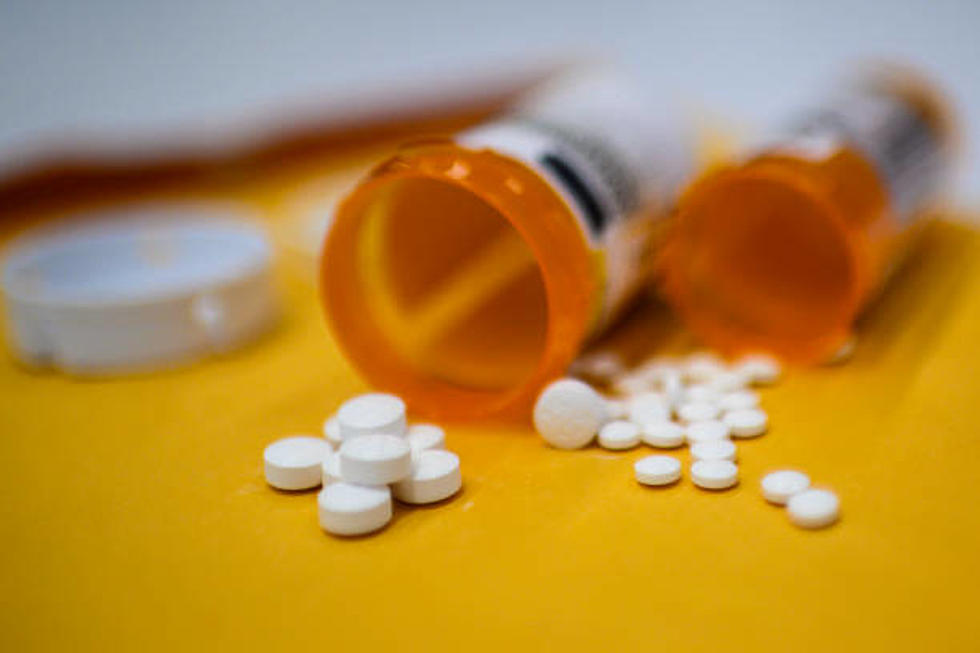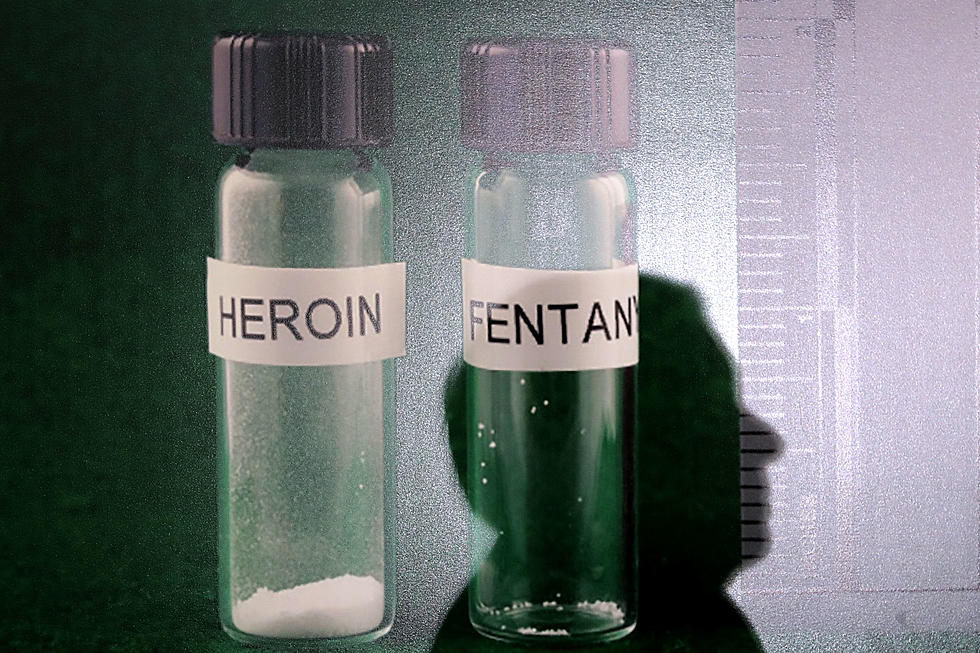
Overdose deaths in New Jersey dropped 8% this summer
Contrary to all the talk about how opioid-related deaths have spiked during the coronavirus pandemic, New Jersey recorded an 8% decline in fatal overdoses this past summer.
Between June and August, there were 754 opioid-overdose deaths in New Jersey, compared with 821 in the same period a year earlier – a drop of 67. Overdose deaths dropped 14% in August and 12% in July, after a 4% increase in June.
“Look, one opioid overdose death is one too many, and so we’re very concerned the overall trends in our numbers. And we always are,” said Human Services Commissioner Carole Johnson. “But it is the case that if you look at June/July/August, compared to comparable months last year, the numbers are trending down.”
The relatively better summer follows a 7-month period that started last November in which deaths had jumped 18% from the same period a year earlier, including the first few months of the pandemic that included its spring peak.
“We had obviously a very tough run there at the peak of the pandemic, but if you look at the February to May numbers for this year, they look not so dissimilar to the summer months of last year,” Johnson said.
“We don’t know exactly what’s driving all of those trends. We often talk about and think about: What does fentanyl look like? What is happening on access issues to some of these things?” she said. “… Our concern is about making sure people have access to treatment and can get on a path to recovery.”
Over the first eight months of 2020, overdose deaths are 8% higher than in 2019 and 3% above 2018’s level. September data should be available around the end of this month.
Johnson said the state has focused on three main areas related to opioid overdoses during the COVID pandemic: funding, access to care and outreach.
“The biggest piece of that has really been telehealth, tele-mental health, being able to access services remotely,” Johnson said. “That’s not the answer for everyone, but it has been proven incredibly beneficial for a number of people, to be able to stay connected to your counselor or to your peer support network for those individuals who are in recovery.”
Johnson said that not all the data is yet available but that anecdotal evidence from the state’s substance-abuse treatment providers shows people who’ve struggled to access treatment in the past because of transportation, work or child-care barriers are more readily engaging in treatment because they can do it remotely.
She said that was possible because of changes to regulations, work with the Legislature, flexibility by federal regulators and payment changes.
“We’d like to see as much as we possibly can stay in place with respect to telehealth going forward,” Johnson said. “We’ll need the feds’ help, but we have seen the benefit of what telehealth can do in this space.”
To ensure mental health and substance use safety-net providers could remain open, throughout the summer the state advanced their payments. It also allocated $25 million from its federal Coronavirus Relief Fund to help them with COVID-related costs for personal protective equipment, testing and facility modifications. It also increased long-term residential rates during the pandemic.
Johnson said the state also worked with federal regulators on other changes, such as allowing some patients to take home more medications for longer periods of time and beginning medication-assisted treatment remotely.
The state also focused on outreach through its 1-844-REACH-NJ hotline, which provides round-the-clock connections to treatment, and it distributed nearly 40,000 doses of the overdose reversal drug naloxone – around 11,000 to EMS agencies and more than 28,000 to the public through pharmacies last week.
“We are worried about a second surge on all fronts, and the ongoing fight about the opioid epidemic is part of that concern and part of our planning,” Johnson said.
“We have to make sure that we don’t lose sight of the fact that we’re losing far too many individuals to opioid overdose, and we need to have as many tools as possible,” she said. “Our goal is to really create the policy/funding/support environment and outreach and engagement to make sure people know there is a place where they can get connected to treatment and that they’re not alone.”
Johnson said the challenge is making treatment accessible early in the pandemic is that people were concerned about being in inpatient, congregate facilities and didn’t realize there are outpatient options.
“Certainly some people need long-term inpatient treatment. But not everyone does,” Johnson said. “And there are many ways and many clinically recognized – in fact, the clinical gold standard for opioid treatment is medication assisted treatment that can be done with your primary care provider. So there are many ways to get services and support that don’t require you being in inpatient treatment, and we want to make sure people know that they could get connected to that kind of treatment.”

READ MORE: American Dream reopens, most retail closed
More From WPG Talk Radio 95.5 FM